As health-care workforce shortages continue to strain communities nationwide, colleges and universities are stepping in to fill critical gaps in care.
From mobile dental clinics in rural Tennessee to student-run rehabilitation services in Connecticut, institutions have expanded access for underserved populations—all while creating workforce pipelines and hands-on learning opportunities for students.
Here’s how four institutions are using health-care education to strengthen communities and prepare the next generation of providers.
- California State University, Stanislaus: Community Health Workers
After the death of her child, Sharee Wilburn Grimes leaned on her mother to help her navigate her grief. As an angel mom—a term used by mothers mourning the loss of a child—Grimes said having someone to guide her through healing made the journey toward acceptance less overwhelming.
That experience eventually led Grimes to the Community Health Worker program at Stanislaus State, an 80-hour course designed to prepare participants for immediate employment connecting rural, underserved communities to health care and social services.
The program reflects a growing effort among colleges and universities to create short-term health-care workforce pathways tailored to regional needs. Launched in 2024, the hybrid program has expanded across California’s northern San Joaquin Valley and includes paid stipends for participants.
To date, nearly 200 students across seven cohorts have completed the training, which prepares participants to help community members access health services, manage chronic conditions and receive preventive care. The program also includes Spanish-language cohorts, representing 26 percent of participants, to better serve the region’s large and growing Latino community.
Nearly 200 students have completed Stanislaus State’s Community Health Worker training program through seven cohorts.
California State University, Stanislaus
Some 70 percent of graduates have found employment within three months, and 78 percent are currently working with community-based organizations, health-care providers, schools or local agencies. Together, they now reach roughly 2,000 community members each week.
Sarah Sweitzer, Stockton Campus dean at Stanislaus State, said the northern San Joaquin Valley is medically underserved relative to other parts of California, contributing to disparities in health outcomes across the region.
“If you look at the ZIP code effect—if you look at somewhere like Irvine, which is very affluent, versus Stockton, which is less affluent—there’s a huge difference in life expectancy,” Sweitzer said. “We know community health workers can bridge that gap. They’re trusted messengers—the go-to neighbor, the go-to church member, the go-to person at a nonprofit—who help connect communities to health care.”
- Meharry Medical College: Mobile Dental Units
Kyla Marks’s grandmother grew up in a small, rural town in Mississippi where access to dental care was scarce—a gap that left her without most of her teeth by her mid-30s.
“When I came into this world and met her, I never really saw her smile,” said Marks, a fourth-year dental student at Meharry Medical College, one of the nation’s oldest and largest historically Black medical schools.
When her grandmother died in 2020, Marks carried that loss with her, determined to expand access to dental care in underserved communities.
Marks is one of more than 300 students enrolled in Meharry’s dental school. Since 2018, the institution has expanded beyond its home base in Nashville, becoming a key provider in rural health-care deserts across Tennessee. Its mobile dental units have delivered care to underserved communities throughout the state. Last year alone, providers performed more than 4,000 dental procedures across Tennessee.
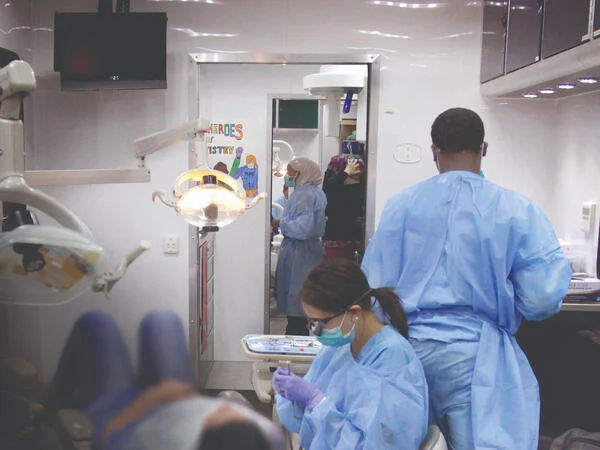
Meharry’s mobile dental units travel to underserved communities, serving as a key provider in rural health-care deserts across Tennessee.
The college has also become a trusted provider in many rural communities, including predominantly white areas that might not traditionally seek care from an urban-based, historically Black medical school. The effort reflects Meharry’s long-standing mission, said Julie Gray, associate dean of external affairs at the college, who leads its mobile efforts.
“Many of our patients are white and they love us no differently—and we serve them no differently,” Gray said. “Teaching our students how to serve people, restore confidence, build trust and patience, is what we do, no matter who the patient is.”
- Quinnipiac University: Accessible Physical Therapy
Each Tuesday from 4 to 7 p.m., Alyssa Campo helps provide physical therapy to uninsured and underinsured patients at a student-run rehabilitation clinic at Quinnipiac University.
Alongside roughly 60 fellow volunteers, the doctoral student works with patients who might otherwise go without care while gaining clinical experience under the supervision of licensed faculty and alumni.
Linda Bedard, clinical assistant professor of physical therapy at Quinnipiac, said the EQUIP Rehabilitation Clinic began in 2012 as a student capstone project and experienced a surge in volunteer support beginning in 2021.
Today, more than 80 percent of the university’s doctor of physical therapy students volunteer at the pro bono clinic while completing a demanding graduate curriculum. Together, they have provided full physical therapy services to more than 400 patients.
Quinnipiac University’s student-run clinic helps physical therapy students build professional identity and a strong service ethic.
Bedard said the clinic gives students sustained clinical decision-making experience, including evaluating patients, developing treatment plans, completing documentation and providing follow-up care. At the same time, it helps students build a strong sense of professional identity and service.
“Our health-care delivery system in the United States really is a struggle for a lot of people who are uninsured or underinsured,” Bedard said. “There were plenty of clients who actually needed our services if we could do it free of charge, so filling that gap has been a win-win for everybody.”
- Touro University: Rural Clinical Training
At a rural clinic on a Native American reservation, Nina Sanfilippo encountered a model of care designed to keep patients—and aspiring health-care providers—rooted in their community.
Sanfilippo, a third-year physician assistant student at Touro University, spent 12 weeks in a clinical rotation in Covelo, a quiet, rural town in Northern California where the closest hospital and medical specialists are nearly two hours away.
Across the country, rural communities face persistent shortages of physicians and dentists, despite decades of policy attention. Sanfilippo is one of many medical students at Touro who are part of the institution’s effort to address those gaps through locally centered training models designed to keep providers where they’re most needed.
Touro has taken a place-based approach in two states—California and New Mexico—using its medical and dental schools to build clinics and workforce pipelines focused not just on training but on rural retention.
Third-year students and faculty at Touro University’s College of Dental Medicine provide care to a patient at the newly opened clinic in Albuquerque, N.M.
Alan Kadish, Touro’s president and a physician himself, has been a driving force behind the institution’s investment in rural health care, choosing to open satellite colleges in rural communities and train providers to help fill long-standing gaps.
“We partner with the local communities where we are and try to understand local culture—the way local health-care systems and government work—and try to interact with them positively,” Kadish said. “It has been a conscious effort, and one that’s needed to make a difference.”
Get more content like this directly to your inbox. Subscribe here.